ABOUT DIAGNOSIS
 |
Autism is a 'fruit salad', a 'straws on the camel's back' scenario. Every person with autism has a different history underpinning their own unique 'autism fruit salad'. I see Autism as 'straws on the camel's back syndrome' and ask myself what contributed to my autism? If someone diagnosed with autism makes a significant level of progress as I have, it is natural to wonder if they could ever have 'really been autistic'.
Whilst we expect many people with Aspergers to commonly be recognised for high IQ or giftedness, when those diagnosed with autism make significant progress it challenges the theories, the assumptions, the one size fits all autism packages and makes people wonder whether the same could be possible for their child, the people they work with.
Someone can also be autistic then experience environmental damage, such as brain injury, that exacerbates the presentation of their autism and once a child is autistic, particularly if they are functionally non verbal, they may, in the wrong environment, be far more vulnerable to being chronically abused because all the impacts and responses may most likely be deemed part of their 'autism' or 'a regression'. This was the case for me.
For this reason I set forth what I have learned throughout my life about my own case. This is not to presume that my case is at all reflective of the 'fruit salad' that makes any other person 'autistic', but, instead to merely demonstrate the Fruit Salad model of Autism including my own lived example of environmental insults that can and did get confused with/contribute to/exacerbate my autism. Here's my complete developmental and diagnostic history:
PRE NATAL

I inherited a rare genetic collagen disorder from my mother's side which has been recently linked to autism and particularly brain connectivity so this would already have effected me prenatally.
However, autism is often the product of many interconnecting circumstances. I was also an unwanted pregnancy of a depressed, heavily smoking, alcoholic teenage mother who still had her first baby in nappies. She had already been a regular heavy binge drinker for 5 years before I was born. Like most alcoholics she likely had poor nutrition. My father was a serious binge drinker but not an alcoholic.
Abortion was not yet legal in 1963. As such, I survived my mother's two home abortion attempts with Quinine (a neurotoxin in excessive doses).
She relayed that during her pregnancy with me my father apparently threatened her with an axe. I have no doubt he was capable of this, that their domestic challenges left her with PTSD, and no doubt she would have experienced a flood of cortisol in this event if not other similar ones during that time.
I was born in 1963 with a birth weight of 2740g (6.0 lbs) and a length of 47cm (18.5") which is the normal length and weight of a fetus at 36 weeks.
EARLY HEALTH:
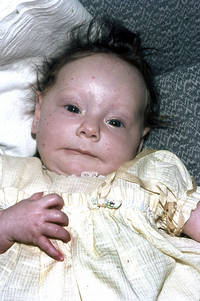
I was delivered naturally. At 4 months old I had measles and at 2 years old I had mumps. By the age of 6 months old, I had chronic Cradle Cap (Sebhhoroeic Dermatitis), Colic, Rickets, associated jaundice and recurrent abscesses and respiratory tract and ear infections. I spent my first 26 years regularly on antibiotics. As a very selective eater until I was 9, I had a very limited diet throughout childhood and primarily restricted myself to the foods to which I had food allergies and intolerances as well as extreme alternating sugar and salt craving.
EHLERS-DANLOS SYNDROME (EDS):

In 2012 I was diagnosed with EDS, a genetic connective tissue/collagen disorder . Collagen is involved in joints, ligaments, muscles, skin, organ development, the vascular system, membranes throughout the body (including the blood brain barrier) and protects nerves throughout the body (those with EDS carry a 10 x higher risk of MS). It plays important roles in brain development and information processing, is an important signaller and regulator at the cellular level. Those with EDS commonly have a history of food allergies, recurrent infections, and a higher incidence of developmental delay/information processing issues. Most people with EDS will have relatives with it (as in my case) but any form of EDS can also occur 'de novo', in a family where it has never previously been seen.
Because collagen is important in blood pressure regulation around 40-70% of people with EDS develop some broader level of autonomic dysfunction associated with blood pressure dysregulation. This can effect respiration, heart, circulation, temperature, bladder and digestion/bowel function and can come with associated dizziness and fainting or near fainting.
There are different types of EDS and one can have features of more than one type. I am diagnosed with EDSIII/IV. Type III effects around 1 in 5000 people, type IV is presently thought to effect around 1 in 40,000. I have four relatives on my mother's side who had ruptures before the age of 40 (two with uterine rupture, one with spleen rupture, one with brain aneurysms) which makes it likely I have type 4 (known as EDSIV or VEDS),
Whilst EDSIV/VEDS is known to come along with significant health risks and most diagnosed with it do not live into their 50s, it is also true that most are only diagnosed once they rupture and so there may be many more who live a normal life span who simply go undiagnosed just as I had. I have the easy bruising and fragile veins but have never had an arterial or organ rupture.
IMMUNOLOGICAL
Collagen plays a role in both brain connectivity and immune regulation. As such, those with genetic collagen disorders commonly also have a range of immune related issues.
When first diagnosed with IgA deficiency in 2001 (it was 'trace', meaning virtually none). Fortunately, it improved to being a more moderate deficiency and eventually only a mild deficiency (partial IgA deficiency). I also grew up with varying levels of neutropenia which I was first told about when I was 17. I was not told how severe it was, just that they took three slides of my blood to find a white cell. In my 30s I was again given the news I was neutropenic, but over time this became only mild neutropenia and sometimes these days I'm inside of the normal range. In 2009 I was diagnosed with the further complication of IgG2 deficiency which may or may not have been there earlier. In 2015 I got a normal IgG2 result so this too may have self corrected.
IgA deficiency commonly comes with a ten fold increase in incidence of celiac, higher rate of allergies and infections, inability to manage the body's natural Candida, poor enzyme production, poor gut immunity and risk of further immune deficiencies. IgA deficiency has also been associated with increased incidence of some autoimmune diseases.
I was diagnosed with IgE allergies to wheat, soy, peanut and told I would have had these since a week old. I was also diagnosed with celiac which I presume I'd have also had all my life (like many with IgA deficiency I had false negatives to the IgA celiac test). I have salicylate (a natural plant toxin) and casein (milk protein) intolerances with severe CNS reactions to cow's milk products. I get sensory neuropathy and gut issues from gluten. I get hives, asthma, gut issues, edema, systemic inflammation and agitation, hyperactivity and hypomania from high salicylate levels. I used to get an LSD like effect from casein in cow's milk products, as well as colic, IBS and headache/migraine and asthma. I get agitated, aggressive, obsessive with wheat as well as IBS. I get brain fog, confusion, and psychiatric symptoms from soy/peanut and some of the legume family.
"Acute pathologies, caused by trauma, metabolic upsets, drugs, and infections, for example, are particularly associated with “delirium” or confusional states, with prominent impairment of attention, while slowly progressive pathologies are more often responsible for “chronic brain syndromes." http://jnnp.bmj.com/content/76/suppl_1/i31.full
My immune, and metabolic challenges may have been inherited or acquired or a combination. People can have these conditions and be asymptomatic. Others in the same family can be significantly more effected. In me, these issues may have been exacerbated by prenatal health in being born to a heavily smoking alcoholic mother and later worsened by my own poor nutrition (extreme neglect in my first six months and later became a selective eater with very limited nutrition until late childhood), untreated food allergies and food intolerances, recurrent antibiotics for my first 26 years, growing up with two heavy smokers smoking in the house, living with PTSD and chronic fight flight until my 40s and living with an untreated hypoventilation syndrome until 2012 - none of these issues would have done my health any favors and the more these issues were addressed the more my status has shifted from immune deficient to simpler low immunity.
CONSANGUINITY:

Consanguinity means shared blood line. My paternal grandmother was the child of what is known as Double Cousins. Double cousins are second degree relatives and genetically equal to half-siblings (sharing 25% of their genes). Her own two grandfathers were brothers and her two grandmothers were mother and daughter. My father, who may have had FASD and fitted diagnoses of dyslexia, ADHD and bipolar, was the last of 7 children, born when both of his parents were in their 40s. He was his mother's 7th child (though all his siblings are half siblings). His mother was a kindly, warm, simple lady and a 'dipso' who was less flatteringly referred to as 'dotty, potty and deaf'. I feel she may have been on the autism spectrum. Whilst inherited strengths would also be multiplied, genetic mutations/birth defects are common in consanginous marriages. In the case of double cousins this may be as high as 15%. Some of this might be expected to find its way further down the line.
FETAL ALCOHOL SPECTRUM DISORDER (FASD):

At present up to 50% of women drink during pregnancy or in the weeks before they knew they were pregnant. FASD is the most common cause of developmental disability. Unlike its more severe relative of FAS, around 70% of those with FASD have few or none of the abnormal facial features found in FAS - they look 'normal'. 80% of children with Fetal Alcohol Spectrum Disorder fit an autism diagnosis.
My father reported that throughout childhood his mother was commonly tipsy or drunk on red wine. It's possible she had drank during the pregnancy with him and that he may have been an Fetal Alcohol Spectrum Disorder (FASD) child and she in turn may once have been an FASD child herself.
My mother prefered to call herself a drunk on the basis that since she was a teenager and all through my first years, she drank quite openly for the purpose of getting drunk. In my early years she was a gin drinker and it was not unusual for her to drink until she passed out. Later, like her own parents, this became beer and through my childhood it was normal there'd be at least half a dozen empty bottles of beer the next morning or a dozen cans. I saw this plain and simple as alcoholism. She was a heavy drinker and and smoker for several years before I was born. Alcohol, Valium and cigarettes had been an ongoing part of her life throughout my entire childhood. I understand from two aunts that it was normal that up to the age of four she would put gin and Valium into my baby bottles to keep me asleep.
My father was a binge drinker and it was not unusual for him to get himself raucously drunk.
Fetal Alcohol Spectrum Disorder results in developmental disability that includes cognitive, sensory perceptual and communication disorders as well as associated health disorders. Many with FASD are diagnosed with autism or ADHD as part of the prenatal damage they sustained as part of FASD. Gerstmann Syndrome had a range of contributing causes, including prenatal alcohol damage and I have dealt with the issues listed as usual in this syndrome.
CARERS:

My pregnant mother moved in with my father and his parents when pregnant with my older brother. I was born 16 months after him. My mother (who quite likely had Reactive Attachment Disorder among other challnges) named me Donna because she was reading the Spanish dictionary at the time and it meant 'female'. When I was around 2-3 years old she developed attachment to me as her Narcissistic Object and called me 'Dolly' and, in her own words she 'owned' me and "I was her doll and if the doll was bad she was allowed to smash it'. Her side of the family, none of whom I had bonded with, also followed suit and called me Dolly. So the names Donna and Dolly, I associate with someone I had no bonding with, my mother.
To my father and his parents who had lived with me since birth, I was never Dolly, nor Donna. I was not seen as a doll at all and was referred to as Polly. Perhaps this was from Pollyanna, a popular 1960 film at the time, or perhaps because I was echolalic, as in being like a parrot. I was referred to as Polly until I lost the grandparents when I was 4 and a half years old. Beyond this my father continued to refer to me as Polly until his death when I was 35 and those who worked with him also called me Polly at his workplace, as did his sisters and my paternal aunt, Rhonda. From age 5-8 years old the dance teacher also picked up on this and referred to me as Polly. So Polly is the name I emotionally identify with.
I'm told by a paternal aunt that my grandmother slept in my room with me until I was three months old so effectively she was experienced as my mother. My (homeless/itinerant) paternal grandparents lived on and off again in a weatherboard shed in our back yard (which I considered 'home' and spent time there daily). They lived there until I was 4 and a half when my grandfather died and my grandmother was sent away permanently the same week. They were warm hearted, kindly people and I was healthily attached to both of them, trusted and felt safe with them. I have wonderful and happy memories of these grandparents and the safety and containment of the shed they lived in, particularly when I was around 2-4 years old.
When I was 3 years old my mother was sectioned as an involuntary psychiatric patient following a shooting incident in the home but was soon released once she convinced the psychiatrist she had merely been reacting to my father's domestic violence. Nevertheless, because of my mother's significant challenges, my grandparents became my legal custodians until the death of my grandmother when I was 7 years old.
I was also in a quite institutionalised 1960s welfare program which at that time (before childcare as we know it today) provided for at risk children on weekdays from 9am-5pm, from the age of 6 months to 2.5 years old. It was in a Victorian building. A homogenous, predictable, methodical and structured environment run by Sister Jellie. Because I was severely faceblind and all the nursing sisters were in the same white uniforms, I experienced them collectively as 'Sister Jellie' but also specifically warmly remember the actual Sister Jellie. I felt safe at this place and thugh it was 'only institutionalised care', this safety was my definition of 'home' and feeling 'loved'.
In our small dead end street I was cared for by and had bonded with an Italian-speaking mother, Mrs Cappellazzo. I have warm, fond memories of Mrs Cappellazzo, her garden, her house, her daughter (2 years younger than me) from around 2 years old but learned from her that from when I was 6 months old my mother had been leaving me through her gate in the pram. Without any English, she had simply taken me inside and cared for me. By 2-3 years old I was taking myself into her garden and I was welcome in her house, remember her hand feeding me, but by age 3-4 I remember her crying and pulling the blind down on her back door, leaving me out there. By age 5 I remember her son, two years older than me, shooing me out of their garden. And so I lost my 'Italian mother'.
At nights I was commonly taken out all night in the car by my father (who would go collecting payments). My father was jolly and warm toward me and I felt safe out with him, felt liked and I liked him. I enjoyed him singing, the car radio, the vibration of the car. On arrival at homes, he'd leave me in the car, sometimes for what may have been hours. I was neither hot nor cold. He would leave windows part wound down or give me his coat as a blanket. I felt safe being in the glass bubble of the car and could see the houses he had gone into.
I also learned from my mother's great aunt, Gladys, not long before she died that I was also regularly left in her care between birth and 4 years old though (to her disappointment) I only remember her from being around 7 years old. Gladys was a no nonsense gritty woman who was funny and had looked after her own (now older) children. I don't feel I bonded with her, but I have no traumatic memories of her, her tiny grungy Brunswick terrace house home, her children and I have certainly got parts of me that identified with her.
So my identity and personality development reflects that I had significant bonding with several of these people before age 4, just never had any foundations to achieve bonding with my biological mother. I describe it as spending my first 4 years in a Kibbutz with several carers who largely had limited relationships with each other and a chaotic, traumatising human being in there somewhere that just happened to be my biological mother. When I think of the concept of family and home, I associate this with my paternal grandparents and being with them in their shed in the back yard of the house I lived in.
When I was 8-10 years old, I was accepted into another Italian family around the corner from my family (which stopped me throwing stones at their windows at 1-2am!) and I considered one of their daughters - who was aged 10 when I was 8 - to be my new mother. I slept in a bunk with this girl and felt the same security I'd have once known with my paternal grandparents.
At school in grade 5 when I was 10 years old and finally moving from echolalia to functional speech I was dealing with bullying and became confrontational, reactive and violent. The following year I bonded well with my grade 6 teacher at age 11 and this stopped me derailing as fully as I might have. By high school at 12-13, however, I was entering homelessness proper. As is usual in kids with FASD, I derailed into substance abuse in until I was 17.
At 13-15, as a streetkid, I was taken in by a single mother and her teenage daughter as a member of their family. I moved between this home and that of three other teenagers who each looked out for me, helped me, and were all like family to me. From 15-25 was an era of 'domestic prostitution' so common for homeless/itinerant girls/women who live with people they don't love and who don't love them to stay 'off the streets'. During these years I experienced kindness, generosity and help from shop keepers and neighbors which gave me belonging.
Though having an attachment disordered mother so easily passes the same on to the children, the healthy experiences with early carers and support in the local community meant any 'attachment disorder related behaviours' were almost exclusively limited to interactions with her. From the time I left home completely at age 15 I had very limited contact with her, and have had no contact since 2001. I have come to terms with who she was as a child, and who she became and this understanding leaves me with compassion tempered with a grounded awareness that she was and is what she is and that ongoing non-contact is the healthiest path.
BRAIN INJURY:

PRE-NATAL
From the accounts of my father and paternal aunt, I understand that my mother had taken Quinine twice before I was born in two consecutive failed attempts to induce abortion.
POST-NATAL
I understand from them that having failed abortion, she was unable to cope with taking me home and simultaneously opposed allowing anyone to pick me up, feed me, speak to me or change me. Her intention, as it was conveyed to me by both my father and paternal aunt, was to 'let it die', essentially to commit infanticide through neglect. However, as she was drinking herself unconscious at that time and my father, paternal grandmother (who all lived with us) and the paternal aunt when present, continued to give me enough intermittent care to keep me alive until professional intervention.
In the 1960s insecticide was sprayed using pump action dispensers. My mother would use this in the kitchen and I remember her finding my avoidance of the spray entertaining and deliberately spraying me directly with it between the ages of 3-6 years old. I can say without doubt that I regularly inhaled insecticide in those years.
At 6 months old, I had been thrown through a window which was around the same time I started in a welfare program for at risk children. I was told as an adult by two aunts that I was regularly given baby bottles with gin and my mother's Valium in the milk to 'keep me asleep' which could have been earlier but would have been most virulent once I left the at risk program at 2 and a half year old and before I was in a kindergarten program at 3 and a half years old. Valium is not for children, has caused SIDS and severe depression of respiratory drive resulting in hypoxia and, essentially greater or lesser degrees of asphyxiation.
I was also knocked unconscious several times. Closed brain injuries can be mild, moderate or severe. They can be clinical with obvious impairment to functioning or subclinical with the person continuing as they were before. Damage may or may not show up on MRI at the time but decades later the MRI may re unremarkable. These were the number of times I remember or know I was knocked unconscious:
Age 11: I went to school with a black eye. No memory of it, just of being questioned by the teacher.
Age 12: I ran at a male visitor to headbutt him but he moved and I ploughed into the wall, knocking myself out cold
Age 13: My abuser hit my head into wall repeatedly until I went unconscious. I remember the first few times my head hit the wall so at least 4 times by the time I was out cold. EFFECTS: woke in a dream and everything was slow and surreal, couldn't remember how self feeding, dress, don't remember using the toilet, stopped speaking, thought I'd gone 'mad' (my abuser told everyone I had had a 'breakdown'). I was off school for 6 months and at some point in that time was sent up the country to live with a relative, returning once I was interacting, speaking etc. However, when re-enrolled (school number 2) I was not the same kid. All classrooms seemed interchangeable, couldn't understand language (was like this to late childhood now like this again), couldn't follow an instruction, sudden volatility and aggression. After 2 weeks I had to be enrolled in school number 3. I couldn't retain what I'd been told or learn from experience, long periods banned from all classes and only supervised in coordinator's office.
Age 13-14: It was common that on returning home I'd be physically abused. There are also two witness accounts of me being knocked out on arrival home (punched in the face/black eyes). Luckily I became so terrified of returning I became homeless instead and have never been unconscious since (except anaesthetics).
I was probably knocked out in years before I was 11 but I wouldn't remember. I know I survived being thrown through a window at 6 months (legal report by aunt) and that at age 4 I was twice thrown at the wall and that the second time I didn't move (witnessed). The GP report read to me in my 20s included repeated abscesses aged 2-4 which we discussed and he agreed this could be from being repeatedly slapped (matches legal report by aunt). Serious physical assaults were less between age 4-8 (because I got enrolled in dance so there was a vested interest in keeping me presentable) and a foster family from age 8-10 helped me stay safer at that age. When this broke down I was again at far greater risk.

OXYGEN STARVATION & HYPOXIC BRAIN INJURY
In addition I was suffocated numerous times from age 2-3 and perhaps as long as up to age 4 as well as strangled a number of times. I clearly remember initially fighting for my life during these episodes and that progressively I found I had no desperation to breathe, so this neurological function had been damaged in this process.
It is of course also theoretically possible that my genetic EDSIII/IV related collagen disorder could have caused progressive degeneration of muscle spindles and stretch reflexes in the lungs which would also ultimately diminish the effective messaging of blood oxygen and Co2 levels underpinning functional respiratory drive.
HEMAPLEGIA
Starvation of oxygen to the brain is the most common cause of pediatric stroke which results in Hemaplegia. Half of all children with Hemaplegia will have psychological problems, including autism.
“Half of all children with hemiplegia have psychological troubles. Some of these, such as autism and attention deficit hyperactivity disorder, may be caused by the brain abnormality.” - See more at: blog.donnawilliams.net/2015/05/01/hemiplegia-and-autism-fruit-salad/
“Half of all children with hemiplegia have psychological troubles. Some of these, such as autism and attention deficit hyperactivity disorder, may be caused by the brain abnormality.” - See more at: blog.donnawilliams.net/2015/05/01/hemiplegia-and-autism-fruit-salad/
“Half of all children with hemiplegia have psychological troubles. Some of these, such as autism and attention deficit hyperactivity disorder, may be caused by the brain abnormality.” - See more at: blog.donnawilliams.net/2015/05/01/hemiplegia-and-autism-fruit-salad/
AUTONOMIC DYSFUNCTION
Autonomic dysfunction, Central Apnea, agnosias, and cerebral salt wasting are all common in asphyxiation related brain injury. A percentage of cases of autism are also due to oxygen deprivation, though usually due to birth complications not intentional medication and suffocation abuse. The chances that my Munchausen By Proxy mother caused not only trauma but a degree of acquired brain injury that added to my presentation as 'autistic' is of course more than possible. It is, however, also the case that a collagen disorder like EDSIII/IV would also bring with it degrees of autonomic complications.

MOTHERS WITH MUNCHAUSEN SYNDROME BY PROXY
75-98% of those with Munchausen Syndrome By Proxy (MSBP) intentionally damaging their child are mothers. These women have combinations of (often undiagnosed) psychopathy, Narcissistic (NPD), Borderline (BPD) and Histrionic Personality Disorders.
The incidence of these in the human population is: Psychopathy 1%, Histrionic Personality Disorder 3%, Narcissistic and Borderline Personality Disorders 6%. It is therefore reasonable to assume that up to 1 in 20 mothers could have a predisposition to MSBP and if their actions neurologically damage, developmentally derail, psychiatrically impair and/or traumatise their child then the children of those 1 in 20 mothers may, theoretically, be more likely to present with a child who may ultimately get a diagnosis of autism or, as in what happened to me, exaccerbating an already existing level of disability. The majority of mothers with MSBP will present as overly loving, overly concerned mothers.
Not nearly as rare or exotic as once believed, around 1-3% of the population are believed to have Dissociative Identity Disorder. Almost all people with Dissociative Identity Disorder have experienced severe and chronic abuse in their formative years. Some will then go on to have children and statistically only 30% of those abused as children then abuse other children. 38% of mothers with Dissociative Identity Disorder (DID) were found to be exemplary mothers. However 16% of mothers with DID were dangerous abusers of their children. Around 58% of those with DID also fit Borderline Personality Disorder. I personally believe that my mother had DID, that different parts of her were psychopathic, narcissistic, borderline, sociopathic, and had various addictions, and that the Borderline part of her committed the suffocation abuse as part of Munchausen Syndrome By Proxy.
TRAUMA:

Extreme emotional dysregulation, inability to filter incoming information leading to sensory heightening and overload, recurrent ear and upper respiratory tract infections, pulsatile tinnitus, episodes of relentless breathing and ear popping Tourette's tics, severe constipation (to the point of vomiting) all contributed to dissociation from my body, impaired identification with my body, and trauma responses to having a body and being expected to care for it. In other words I believe I felt traumatised by parts of my own 'autism' and that abuse exaccerbated that. Together with the further trauma of loss, neglect and abuse, these other sources of trauma all contributed to a chronic fight-flight state of involuntary avoidance, diversion and retaliation responses I call Exposure Anxiety.
Around 2-3 years old, I was being tied to the bed, locked in my room, slapped repeatedly across the face and beaten with a strap (and hit once across the back with a lump of wood). I have clear recall of a series of assaults when I was around 2-3 yrs old which involved waking to being suffocated with a pillow and sometimes suffocated and choked. Obviously, I survived, but documented in my first book Nobody Nowhere that I took to then sleeping under the bed to escape this abuse. A paternal uncle also gave an account of witnessing me at age 4 being twice flung at the wall. An MRI of my back in 2012 showed old damage to two of my lumbar vertebrae which may have been done at that time. In my 20s I saw my childhood GP and heard that my records showed I had also been examined for sexual abuse at this age (there was no mandatory reporting then) and have no memory of any other abuser at that age other than my mother.
I could more easily come to terms with the neglect and physical, emotional and psychological abuse, I did eventually come to terms with the sexual abuse and understand it in the context of having a mentally ill substance abusing parent from a background of incest. Most abuse of children is at the hands of a family member. Abusers can be anybody, even a parent on the autism spectrum themselves. Children are abused in all kinds of families whether they have disabilities or not. I just got unlucky. But I also got incredibly lucky. I was blessed to also have had a range of healthy carers before the age of 4, a privilege most abused children have never had. The tragedy is that in spite of this my mother was allowed to continue to abuse me until I left for good by the age 15.
HYPOVENTILATION:

I had a number of episodes before the age of 3 where I was described by my father as 'blueish'. At around 2-3 years old I was rescued from the bottom of swimming pools, once at the City Baths and rescued by two old women, once at a motel pool where I was rescued by my older brother. I was an extreme breath holder, able to go without breathing longer than any child I knew. In mid childhood I swam the 100 metres length of the Olympic pool at Preston Baths along the bottom. I came up dizzy but undistressed, having greatly worried those in charge of me there. When I gained functional speech by late childhood and became fluent by my teens I asked 'why do other people's brains keep them breathing and mine keeps forgetting'. This was not understood so not followed up.
As an adult, following 7 months of Haemophilus infection, these daytime episodes progressed and I was waking at times to find no respiratory drive and I was dizzy, had a headache and was not breathing. During chemotherapy two years later this progressed and was diagnosed as part of a wider picture of broad autonomic dysfunction but the oncologist concluded this was not caused by the chemotherapy, but that for some reason I had had this autonomic dysfunction all my life and that chemo was just exacerbating it. A few months after chemotherapy it was diagnosed as moderate-severe Mixed Apnea and progressively since 2012 a ventilation machine (ASV) does my breathing for me during sleep.
In the absence of brain tumor or head injury, other causes include severe viral and bacterial infections which may have been particularly more possible in a context of primary immune deficiencies. However, the other cause of acquired hypoventilation is asphyxiation - autonomic nervous system damage caused by oxygen deprivation.
"Brainstem infarctions and ischemia can result in central hypoventilation syndromes. Watershed infarcts in the brainstem tegmentum in the human fetal and neonatal brainstem can present with multiple cranial neuropathies, central hypoventilation and apnea....viral encephalitis can also occasionally result in central hypoventilation". (from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2885790/ )
"Impairment of vision may occur due to infarction of watershed zones in the posterior cortex. This can manifest as cortical blindness and Balintsyndrome (ocular apraxia, optical ataxia, simultagnosia). Cognitive disorders following HIBI are most exhaustively studied sequelae. The selective vulnerablity of cognitive areas results in a wide range of disorders, ranging from disorders of consciousness, disorders of behaviour, mood and affect, impairment of attention, memory dysfunction execution of sequential tasks, etc. Recovery, though variable is to be anticipated over one or two years." (from http://medind.nic.in/icf/t11/i2/icft11i2p65.pdf )
Given my mother a) had twice attempted abortion using Quinine (known to cause nervous system damage in the fetus) and b) in my first years was being drugged with gin and Valium (probably most virulently between age 2-3) and c) that I had experienced several non fatal episodes of suffocation and choking at that same age, it is relatively imaginable that I may have sustained hypoxic damage to my autonomic nervous system from this series of events. If so, this original level of damage could later have been pushed further following a long term respiratory infection, chemotherapy and surgeries to eventually leave me with depressed respiratory drive requiring ventilation to keep breathing during sleep. However, in the last few years research in the fields of both autism and Ehlers Danlos Syndrome have explored autonomic dysfunction and there is a reasonable possibility that autonomic dysfunction would have happened anyway, it was merely exacerbated by other events. With EDS having a 10 x increased rate of MS and MS being one of the conditions in which failed respiratory drive does occur, it is possible this highly unusual progressive complication was genetic and ultimately inevitable.
SLEEP DISORDERS


Healthy sleep-wake cycles, adequate REM and healthy, unfragmented sleep are all essential to brain development, mental health, learning and physical health.
I had extremely disturbed development of sleep-wake cycles and a variety of sleep related disorders.
- Though my father's mother had slept with me from birth to 3 months old, from 3-6 months old I had been kept in a dark room with a blanket over the window.
- From age 2 and a half to age 4 I was given gin and Valium and commonly kept asleep indoors during the day. The suffocation abuse and strangulations visited upon me by my mother in the night left me terrified and entirely unable to trust sleep.
- Like many with EDSIV I slept with my eyes open until late childhood.
- At our second house, from age 7-15, I was extremely light sensitive so during the day I would close the curtains to keep the room as dark as possible. At this house I also would not sleep in a dark room so there was always a light on until I was into my teens.
- At the second house, my substance abusing parents through large, rowdy parties most weekends. These were often dangerous and endangering. It was common to wake up to strangers in my room getting tours of the house and there to see the view across the city (I slept in an attic). It was also not uncommon to wake in terror to the sounds of domestic violence and need to take immediate action. It was therefore not unusual for me to escape to the safety of the streets in the early hours of the morning. As such I found myself another family around the corner at 8 years old so until I was 10 I finally got some sleep around there!
- At around age 11 I was put on 'sedation' which made me all the more endangered within that house. I began to have night terrors, sleep walking, sleep talking, bed wetting. I stayed on these sedatives until I was 17 when I wanted to feel 'awake'.
- When I came off sedation I began violently striking out in my sleep. This eventually stopped. From my 20s-30s I experienced isolated episodes of sleep paralysis, hypnopompic hallucinations and eventually PTSD nightmares.
- Not surprisingly from this background it was usual for me to not sleep until 1-2am and be up at 6-7am as my 'normal'. This finally normalised in 2001 at the age of 38 when I went onto medication - Seroquel 50mg for chronic fight-flight, reduced to 25mg 2010 and not required since 2011.
- I had 'zoned out' all my life but in 2012, aged 49 I developed sleep attacks that in 2016 were diagnosed through MSLT as hypersomnia/narcolepsy with underlying sleep fragmentation. This became managed with Gabapentin but microsleeps (likely life long) remained.
EARLY INTERVENTION
 |
From 6 months old (early 1964) until 2 and a half years old (early 1966) I was in a Community Welfare run program under the care of Sister Jellie. In the 60s, it was called Northcote Day Nursery, was one of only 8 Day Nurseries in Melbourne, was government funded, required a referral from a social worker and served at risk children. The children were there Monday-Friday during working hours and home weekends. Today it is a typical modern day care centre with no direct connection to Welfare services.
Kanner did not diagnose children with Autism. For Kanner, autistic was an adjective used to describe the emotional withdrawal and encapsulation of children with 'childhood psychosis' and use of the term remained that way until the 1970s, in some places until the 1980s. Then the psychiatric model (of mad children) became replaced with the cognitive model (information processing disorders) and autistic children were no longer diagnosed as having Childhood Psychosis. The associated adjective had been promoted to take the place of the noun it once described.
Around 1965, aged two and a half, I was diagnosed as psychotic after a three day hospital observation at St Elmo's Private Hospital in Moreland, Victoria. According to my father I had been admitted to determine whether I was deaf (I had no blink response to loud noises), whether I had leukemia (I had repeated infections, was extremely pale, bruised extremely easily, had bleeding gums and my eyelashes came out in clumps) and why I had no pain response (I had had a combined stomach tensing and compulsive coughing tics - part of Tourette's - that compelled me to cough against this resistance so repeatedly that I was coughing specks of blood).
PRESCHOOLS & PRIMARY SCHOOL:
 |
Around 1966, I attended a creche at the Royal Women's Hospital in Carlton when I was around 3 years old. Perhaps because my mother had been sectioned around that time. Perhaps because it was a follow on from the diagnosis at St Elmo's.
From 3 and a half to 4 years old I was at a private kindergarten called Gilmer College in Preston which had a reputation at the time for taking children with special needs.
I began at a mainstream inner city primary school in 1969 and after the first week was selected for a specialised class. It was called the Country Infant Room, designed to teacher city teachers to teach in small country schools. It took only 6 children my age (22 children in total) and involved having the same teacher and same classroom for 3 years.
Throughout primary school in the 70s, I was regularly assessed by Psych and Guidance teams (school psychologists) and learned that, like Temple Grandin once was, I too had been assessed as emotionally disturbed.
THE WORD 'AUTISM'
 |
With regular ear, nose, throat, lung infections I was intermittently tested for deafness until age of 9 when my language processing disorder was finally understood. This diagnosis was reconfirmed in my early 40s by audiologist, Dr Leslie Tan.
In 1973, when I was 10 years old a teacher (who taught at Thornbury Primary school at the time) named Christine had been at one of my family's 1970s parties. Fleeing the violence that erupted there by the early hours, she found me in the street in my pyjamas. She beckoned me into the car and took me home overnight. According to my father, after returning me the next day, she had raised the word autism with my family. Though I'd already been diagnosed as psychotic at the age of two, the actual word 'autism' was not used then because autism was synonymous with 'childhood psychosis' at that time. By the time childhood psychosis was being reworded as 'autism' by 1973, saying 'your child is autistic' was a very accusative thing to say to a mother. The first popular 'autism movie' had come out in Australia in 1971, an Elvis film called Change of Habit (1969) in which the girl's autism is attributed to suppressed rage at her mother (psychoanalytic perspective still common in some parts of Europe today). In spite of this teacher's suggestion, I continued to be more conveniently referred to as 'disturbed' until my 20s when my original diagnosis as 'psychotic' at age 2 was now reconfirmed but with the more modern term of 'autistic'.
ACQUIRING FUNCTIONAL SPEECH
 |
I was 9-11 years old when I progressively went from 90% meaning deaf and predominantly stored phrases, TV scripts and echolalia to being only 50% meaning deaf and finally striving to string simple novel sentences together. By age 11 I could construct slow, klunky simple sentences (and still also had fluent, expressive echolalia), by age 12 I could do long litanies at people and was developing simple conversing skills. By 18 I had learned to suppress much of my echolalia, keeping my 'self chatter' for when I was alone. So how did this happen?
Around age 9-11 my father left a record player and a pile of old 78 records in my room featuring a vast array of theatrical songs from the 1920s-1940s and I came to sing in a vast array of voices with far expanded, albeit echolalic, vocabulary. This also greatly improved my confidence with verbal speech and my enjoyment of it and countered many an episode of Selective Mutism as I progressively moved into functional speech.
Around age 9-10 I was also left a typewriter in my room. I was highly anxious and suspicious of it but I loved pressing buttons and began to type letters. One day there was paper in it and the letter typed onto the page. Over time I overcame my anxiety of seeing myself expressing myself on a page and typed letter strings, then later typed words I knew, then eventually lists of words, then by age 13 was typing poems. This created awareness and confidence in myself as someone who was in charge of flexible, personal and emotional communication through words.
Around age 9-11 my mother mirrors an entire wall in our living room and in my bedroom with mirror tiles. A beaded curtain on the pantry door was also put up between the pantry and the kitchen where people gathered and loving beaded curtains meant I'd stand in it making it clack-clack for extended lengths of time. All of these meant I stayed in the living room and kitchen for greater lengths of time, more exposed to communication around me and spent more time chattering away at my reflection in my room.
My younger brother was 6 years younger than me and by age 2-5 was my closest social contact in the home to whom I had deep attachment. At age 3 he had 6 words, none of which were understood outside of the family. By age 4-5 he was speaking fluently. I would have been 10-11 years old. Being challenged to communicate by a younger child who is moving into fluent speech would have helped me to make a communication leap.
From age 8-10 I made friends with an older Italian girl around the corner and ultimately spent many of my days and nights there, progressively gaining Italian. When I came to speak fluently in front of my mother in functional speech it was not in English, it was in Italian. This acquisition of Italian was in part due to this environment causing none of the chronic fight-flight at home, the fact I'd had my first 3 years exposed to fluent Italian, the fact that talking a different language allowed me to feel more confident and less prone to being further sabotaged by Selective Mutism, the fact that I was striving for belonging in this Italian family, and the fact the language sensorily appealed to me and had none of the trauma associations that my failures to acquire functional English did.
Around age 9-10 I was diagnosed with severe language processing disorder. This meant I was finally treated as something other than just 'psychotic' or 'disturbed' and my mother began to use slowed, clearly spaced telegraphic speech, augmented with associated gestures and representational objects. This allowed me to not only build up the one-word = one-meaning system (semantics) but progressively understand at least preconsciously that I could also start to combine these.
Around age 10 (1973) I was also put onto Zinc, vitamin C and multivitamin-minerals and, with the help of being sent off to eat along with the mirror, I finally moved onto eating whole meals. It may be I was one of the first people with diagnosed with autism known to be treated with vitamin therapy.
Around age 10-11 I was put on antiinflammatories for juvenile rheumatism (after regularly body slamming my arms and shoulders and punching my legs) and sedatives for chronic anxiety (which I remained on to age 17). It is possible these both helped me gain enough sleep to build new connections and synthesis information I hadn't yet done. I was diagnosed decades later with sleep fragmentation and associated hypersomnia/narcolepsy which I believe I'd had all my life from brain injury. Anything that contributed to me having relief from chronic fight-flight and gaining sleep may have helped me develop communication.
When I was 10 years old, in grade 4, my reading teacher realised I could read fluently but had virtually no comprehension of my reading at all and was only guessing at the meaning of what I'd read. In spite of my distress, disgust and outrage at my demotion to picture-word dictionaries this was a major breakthrough. When she found I could learn these associations by rote but not apply them to the real world she began to use associated gestures. As she did this, having been exposed to this by my father since age 2-3 and by my mother from age 9-10 I now began to convert the pictures into gestural signing and build up the associated words for each experience.
When I was 11 years old, my grade 5 teacher, Helen Elmer, insisted that I use words if I wanted a chair. In spite of my warning glares at her and her awareness I was already labelled 'disturbed' and had no problem living down to that with violence, she was determined to do an 'Annie Sullivan' on me. We had a show down and I conceded. With extreme and slow effort I cranked out with the help of augmentative gestural signing, "I-want-chair-here". She then said, "ok, go get yourself a chair". I got my chair and overcame my rage at her as she continued to encourage me I could create sentences to have my needs met.
As I acquired functional speech the foreigness, klunkiness, slowness of my speech sounded so foreign to me it was aversive. As such I didn't feel pride in it, failed to personally identify with and saw it as not 'natural'. I missed the fluency, ease, emotional expressiveness and many voices of my echolalia and saw functional speech as a poor substitute. Dealing with abuse and bullying contributed to my necessity to gain functional speech but also sent me regularly into episodes of Selective Mutism for days, weeks or months. My father was the catalyst for keeping me communicating though his impromtu singing, his silliness, surrealism and relentless cartoonish provocation.
Aged 11, my grade 6 teacher, Mr Frank Ryan, learned that if he sat in front of me I went Selectively Mute or my language trailed off into echolalic self chatter. He learned that if he sat alongside of me, not looking at me, and used self chatter, I could respond with my own in comprehensible speech. This taught me that I could communicate far better if my listener was clearly in their own space, not watching, waiting, wanting and using less to get more.
By my first year in high school, aged 12, I was communicating in one sided fluent litanies. I could talk at and in front of people but had limited capacity to talk 'with' others. Unfortunately, I had a head injury by the end of this year when my mother hit my head into the wall multiple times until I collapsed. After that I was in a very regressed state and my memories of that time are dreamlike and fragmented. For 6 months lost my capacity to communicate. I was in a dream state, other people's speech was incomprehensible again and 'miles away' and I could not find any thoughts or feelings to express. I was sent off to one of my mother's relatives in the bush who was told I'd 'had a breakdown' and this story was continued throughout my time with that family. Only with progressive neurological complications decades later as an adult have I been able to talk about this as abuse related head trauma. When I returned to school it was a new school. I had had nowhere near the abilities I'd previously had and lasted 2 weeks. My third high school also found me so unmanageable I was banned from most classes and looked after much of the time in the co-ordinator's office - who was later the MP Caroline Hogg. At this school I gained an unofficial foster family and eventually regained the skills I'd had before the head injury.
At age 18 I had limited literacy but was encouraged to return to education in a teriary orientation program. I was given remedial classes and gained progressive literacy and proficiency as a writer. Alongside this I had continued as a poet. By the end of university I had the foundations of being a writer. At 26 I wrote my first book, the first of so many. The success of that book brought me over 100 interviews and these dramatically honed my communication skills, challenging me to learn how to both express and track my speech in order to fluently make comprehensible sense to others. With the help of educational psychologist Dr Lawrie Bartak, I learned how to turn take, giving people time to speak and striving to respond comprehensibly on the same theme.
At 32 years old I gained the capacity to simultaneously process self and other for more than 30 minutes. This allowed me to finally understand the difference between talking 'in front of' or 'at' others and what it was to talk 'with'. I said of this life changing experience, "I have touched the heaven of shared 'social'...I know what it is to be 'with'".
LIST OF INTERVENTIONS
Among the interventions that significantly improved my adjustment and potential were:
- a variety of warm consistent carers before the age of 4,
- fairly regular respite in a range of settings since infancy which developed flexibility and adaptability,
- a father who was great at both an indirectly confrontational approach and as a physical teacher,
- animals as peers since infancy,
- an indirectly-confrontational approach that helped me around some of my Exposure Anxiety,
- swimming and intensive ballet from age 3-8 as brain gym,
- mirrors for communication and socialisation,
- TV, the telephone box and record players and records for extensive echolalia,
- addressing gut, immune, metabolic disorders and allergies,
- being put on supplementation in late childhood,
- gestural signing, slowed/telegraphic speech, representational objects,
- a typewriter for typed communication,
- paints and a pianola and piano which later honed safety with interactive non verbal self expression,
- beaded curtains and cuckoo clocks that kept me from dissociating too far as I wandered in a sleepwalking state,
- attending a mainstream and all the sink-or-swim and survival and modelling in that,
- a 5 years younger brother who brought out the older sister/teacher/peer in me,
- an older brother modelling what a non/less autistic development looks like
- an older brother who hated having a 'spastic' sister so I became aware of what bigotry was and how I had to strive for self management or deal with the consequences,
- colored light bulbs/cellophane/colored glass and later tinted lenses which taught me what cohesive visual perception could be,
- a local community which was inclusive and accepting and allowed me to wander freely within their premises and houses,
- parents who had more challenges than I did so were incapable of babying me or training me in dependency and even at my most dysfunctional I was still a relative 'success',
- being kept fully responsible at all times for my own self management and regularly in sink-swim survival situations all my life so I had to learn to avoid the discomforts nobody else was going to rescue me from,
- a great and relateable teacher in grade 6.
- striving to survive a mother with Munchausen By Proxy who simultaneously deliberately exacerbated my autism and determined I'd either learn to self manage or be institutionalised,
COGNITIVE TESTING AT AGE 26
In 1965, my diagnosis at age two of 'psychotic' came about through three days observation in a hospital. There was probably no cognitive testing at that time. The diagnosis would likely have been purely observational. In 1991, now in my 20s, I had enough skills to participate in formal testing which ascertained my strengths and deficits and whether these indicated the kind of information processing patterns seen in people with autism. This was done by educational psychologist Dr Lawrie Bartak, one of Australia's leading autism experts, from Melbourne's Monash Medical Centre at Monash University. He also spoke with and met with those who had had significant involvement with me as a child. I spent 16 months seeing him regularly as a therapist and also met with a team of his colleagues and students at the Monash Medical Centre and allowed them to extensively question me about my experiences. With 40 years experience in the Autism field, Dr Bartak was recently awarded Autism Victoria's Exemplary Service Award in their 2008 Autism Recognition Awards.
 |
I did not approach Dr Bartak for a diagnosis. I sought to meet others with autism, particularly those who like me had been assessed as psychotic or disturbed as toddlers in the 60s, most of whom were institutionalised in those days. He told me he could help me so I met with him at the Monash Medical Centre. I was surprised when his version of helping me was to do cognitive tests. My IQ was apparently under 70, in the range deemed mildly mentally retarded (yes, I already had an Hons degree and was doing a Dip Ed). However this was made up of extremely high scores on some tasks (pattern related abilities non-autistic people usually don't have), extremely low one's on others (associated with visual and verbal processing). I asked what his tests showed. He told me they showed him I was autistic. I asked how could he be sure I wasn't just crazy. He said a crazy person wouldn't produce these kind of results. In other words, this professional reconfirmation of my autism was accidental.
 |
DID HE MEET ANYONE WHO'D KNOWN ME SINCE CHILDHOOD?
Dr Bartak met with the Paternal aunt who had been deeply involved with me since birth (she was the one who was going to adopt me, had fed and changed me since birth and was regularly involved with me until I was 15, so she was fairly reliable to discuss my history). He also spoke extensively with my primary school teacher, Mr Frank Ryan, who by then had become Principal at the school he was teaching and managed special needs for his region. He also met with Mrs Pauline Turzi (previously Pauline Cowie), the wife of my father's best friend, Bill Cowie. Pauline had known me from age 7-13 and often saw me weekly or monthly during these years. She insisted that I "didn't speak". I knew I sang and did advertisements and long strings from TV shows, so contested this. She replied, "yes, you muttered to yourself but we couldn't understand you".
I grew up dealing with severe abuse at the hands of a personality disordered alcoholic who may have had some elements of AS. As such, I had left home into homelessness by my teens and had obvious Post Traumatic Stress Disorder in addition to my autism related challenges, Because there were others he could interview about my childhood development, learning and behaviour, Dr Bartak had no reason to meet with my abuser. My father, who had not abused me, lived 3 hours from Melbourne and died before Dr Bartak could meet him. Dr Bartak did later meet my brothers.
 |
DID MY FAMILY AGREE TO MY PUBLISHING NOBODY NOWHERE?
Before publishers could publish my first book, Nobody Nowhere (which is a detailed account of my early history and childhood) I had to have "quit claims" signed by all adult members of my family who were featured in that book. This required them to receive a copy of the manuscript to read and sign a waiver agreeing not to legally contest the publication. If they wished to block the book's publication they need only have refused to sign the quit claims. Quit claims were signed by my mother, my father and my older brother, meaning that all had read and accepted my right to publish my account.
Signed written interview testimony was also gathered from my aunt about the validity of my account as well as a friend of the family who had known me since I was three years old and both were gathered by the lawyer at the time and are kept as legal records of the validity of my account.
OTHER AUTISM PROFESSIONALS WHO HAVE PERSONALLY SPENT TIME WITH ME
I have met autism experts and leaders in the field the world over. Among these have been Bernard Rimland, Lorna Wing, Judith Gould, Pat Howlin, Rita Jordan, Tony Attwood, Doug Biklen, Rosemary Crossley, Patrizia Cadei, Adam Feinstein .
The first person to have read Nobody Nowhere was Dr Sebastian Kraemer, a Consultant Child and Adolescent Psychiatrist at the London hospital I was temping at in 1990. The manuscript made no mention of autism and was originally titled "Dolly; Autobiography of a Disturbed Child". I picked him at random, wanting any child psychiatrist to finally tell me 'what kind of mad this was'. He passed it on to his mentor, Francis Tustin, a pioneering psychotherapist and author who worked with those with autism from the 1950s onwards. Francis Tustin passed the book to her publisher who sent it on to UK agent Hilary Rubinstein around 1991 from where it went on to become published as an international best seller.
 |
'FRUIT SALAD' IN MY FAMILY
ADHD, Dyslexia, bipolar, Aspergers and autism have all been diagnosed on my father's side of the family as does Coeliac and diabetes. My father had literacy problems, his usual mode was hyperactive, hypomanic, flighty and exuberant. He had brief episodes where he resembled Gene Wilder as Willie Wonker and with flashing eyes he would tell you he was Elvis or Jesus, that he could cure cancer or hypnotise animals. At other times he would become darkly crazy like Jack Nicholson in The Shining. He was medicated with Valium and Tryptanol so mood disorder goes without saying. He was classically ADHD, had difficulty with reading and writing, had idiosyncratic speech (as did his mother), and likely had some degree of language processing disorder he disguised well with being an animated chatterbox. Though he spent his entire life being extremely outgoing, his letters to me reveal him more as a 'closet schizoid'. He died at 59 from cancer of the pancreas, liver and bowel.
On my mother's side there is an inherited connective tissue disorder called Vascular Ehlers Danlos. On that side is also Obsessive Compulsive Disorder, Agoraphobia, addiction and alcoholism, depression (and several suicides), rage and a vast history of ulcerative colitis and a strikingly high cancer rate (particularly bowel cancer and lymphoma). One of my cousins has a son who is diagnosed with autism and my mother has some features common to Asperger's. She was the second child born to teenage parents (her mother was 14 with the first child) and grew up as one of 8 siblings. Both parents were alcoholics and itinerant until her teens when they got council housing. Incest had been disclosed by at least two of her (now deceased) siblings. My mother was sectioned (involuntarily taken into a psych hospital) when I was 3 years old but was released. She formed a very different relationship with me to that of my brothers. I experienced my mother as akin to the characters played by Michelle Pfeiffer in White Oleander and by Glenn Close in Fatal Attraction . I found myself another home when I was 8, then another when I was 13, left home at 15 and often had no contact with her for years at a time, and none at all since 2001. In keeping with a treatment plan for Post Traumatic Stress Disorder (PTSD) this will continue to be the case. I never bonded with her, hence feel no loss in this disconnection, nor do I feel animosity toward her. I do, however, have very fond memories of the carers who I did bond with.
We are each shaped by our genetics and our experiences, by those we bond and identify with and those we fail to bond with or even the nemeses we identify against and survive not because of but in spite of. As a Taoist, I have no regrets that I came from such remarkably strong personalities with all their associated strengths, weaknesses and challenges.
COMPLETE LIST OF MEDICAL INFORMATION
 |
In addition to language processing disorder and autism other diagnoses over the years included
CHILDHOOD
IMMUNOLOGICAL
- to 6 MTHS (1963): Signs of Rickets , Jaundice, Colic, recurrent infections (recurrent infections and regular antibiotics continued to age 26).
- YRS (1966): Contracted measles and mumps (no MMR in those days) at age 2. In my 30s I was diagnosed (again) with measles which returned and flare up every 6 weeks for 10 months. I'm told I had probably never rid them since childhood and that finally my immune system was beginning to try and clear the virus from my system.
NEUROLOGICAL
- 2 YRS (1965): In a 3 day hospital assessment at St Elmo's Hospital, Moreland - tested for but cleared of Leukemia (extremely pale, bleeding gums, losing eyelashes, extremely easy bruising) and deafness, diagnosed instead as Psychotic (Autism was deemed Childhood Psychosis in the 60s). This was primarily on the basis of what was probably Simultagnosia with associated Verbal Agnosia and Faceblindness in a further confounding context of Tourette's. Some of this presentation would have been due to FASD, some due to Munchasen By Proxy related suffocation abuse at the hands of my mother with the bruising and bleeding gums common in the genetic conditions of Ehlers Danlos Syndrome which can also have developmental effects.
- 2-3 YRS (1965-1967): Cyanotic episodes associated with breatholding when over tired and in terror.
- 3 YRS (1966): Near drowning twice, once at the City Baths (rescued by two old women), once at a motel swimming pool (rescued by my then 5 year old brother), each time just sunk and made no attempt to strive to breathe.
- 9 YRS (1972): Tested for deafness again in late childhood. Diagnosed with Language Processing Disorder.
EDS RELATED
- 7 YRS (1970): Had tonsils out due to crowding (common in Ehlers Danlos Syndrome) and recurrent tonsilitis (common in IgA deficiency) and four teeth removed to allow my remaining teeth to even out as I was growing.
- 9 - 11 YRS (1972-74): was the second shortest girl in my school at age 9 so was put on zinc, C, multivitamin-minerals. As a result of grew to normal height (5ft 1") by age 12 though with associated severe bone and joint pain. Then diagnosed with 'Juvenile arthritis' (common early misdiagnosis in Ehlers Danlos Syndrome) and put onto pain killers/anti-inflammatories for the next 6 years.
PSYCHIATRIC
- 5 - 11 YRS (1969-1974): Assessed as 'Disturbed' by visiting Psych and Guidance team at Primary School (on school records - understanding of autism in the 70s was shifting from 'infantile psychosis' to 'emotional/behavioural disturbance').
- 11 - 17 YRS (1974-1980): Sleepwalking, night terrors, bedwetting, chronic anxiety (all usual in PTSD and also in FASD). Medicated for the anxiety.
 |
TEENS-ADULTHOOD:
IMMUNOLOGICAL
- 17 YRS (1979) First time doctors made me personally aware of diagnosis of having white cell deficiency and what this meant (by my 40s this was only mild)
- 25 YRS (1989) Diagnosed with salicylate and phenol intolerance, severe casein allergy,and multiple food and chemical allergies (including wheat, rye, soy), reactive hypoglycemia, magnesium deficiency.
- 38 YRS (2001) Diagnosed with gluten intolerance. Went gluten free.
- 38 YRS (2001) Diagnosed with IgA deficiency (0.13) (common in those with Celiac).41 YRS (2004) Lost vision in one eye for 3 months. Optic Nerve was ok so conclusion was an inflammatory complication of flu, also found to have Epstein Barr Virus (EBV/Herpes 6) antibodies.
- 46 YRS (2009) Diagnosed with Haemophilus (lasted 7mths), IgG2 deficiency and low blood levels of vitamin D (in spite of sunshine, vit D supplements, omega 3s and a diet rich in chicken/fish). After 7 months overcame Haemophilus then put on prophylactic Doxycycline 50mg (also has good indications in EDSIV).
- 47 YRS (2011) Diagnosed with breast cancer and underwent double mastectomy (no reconstruction) and chemotherapy. I had acute episodes of autonomic dysfunction (pre-existing since my childhood but exacerbated by medically induced sudden menopause and chemotherapy).
- 52 YRS (2016) diagnosed with incurable metastatic breast cancer.
NEUROLOGICAL
- 18 YRS (1980) A psychiatrist who has known me for 2 years observes me in an unfamiliar environment and notes that I have Visual Agnosia. This is the first time my 'meaning blindness' has been explained to me.
- 23 YRS (1986) EEG showed atypical epilepsy (described as a 'highly marked central abnormality'), dx'd as 'Atypical Epilepsy'.
- 26 YRS (1990) Early childhood diagnosis of autism reconfirmed by autism expert Dr Lawrence Bartak, Monash Medical Centre.
- 28 YRS (1992) Diagnosed with a visual perceptual processing disorder. Therapeutic tinted lenses improved visual processing time allowing cohesive processing of visuals.
- 43 YRS (2006) Mid childhood diagnosis of Language Processing Disorder reconfirmed by audiologist, Leslie Tan
- 2012-2016: Diagnosed by sleep clinic with moderate-severe Mixed Sleep Apnea/impaired respiratory drive which responded well to VPAP and 5g sodium per day.
- (2012) Formally diagnosed with Tourette's (present from age 2 and left following Estrogen blockers for breast cancer and menopause)
- Transient brief episodes of sensory neuropathy diagnosed by neurologist with considered caused by celiac (had returned to gluten due to false negative on a celiac test in 2010) and aggravated by the herpes simplex 1 virus.
- Had an autonomic episode with grogginess so slept for an hour. Woke with sudden diplopia. MRI normal. Prism glasses prescribed 12 mths later when still not resolved. Hemifacial spasm was evident in a photo from age 3 and diplopia in photos aged 3 and 4 so the diplopia most likely merely reappeared suddenly.
- Idiopathic Hypersomnia diagnosed following overnight sleep study and MSLT. Cause was sleep fragmentation with 50% reduced REM. Managed with Gabapentin.
- Diagnosed with 'foot drop'. MRI clear. Started Baclofen for severe nocturnal onset stifness and muscle spasms (progressive since 2012) including in the associated leg. The foot drop then progressively recovered 2 months after onset. Returned months later, indicating it was an incidental finding of a pre-existing condition, probably from childhood.
- Two generalised nocturnal seizures were witnessed. Recent MRI clear.
EDS RELATED:
- 36 YRS (2000) keyhole surgery to remove ovary lead to discovery of profuse abdominal adhesions (adhesions common in Ehlers Danlos Syndrome IV). I had open surgery to remove the ovary and correct the adhesions.
- 2012-2014: MRI of the lumbar spine. Diagnosis was Degenerative Lumbar Spinal Stenosis (common in EDS).
- During investigation of my dysautonomia, was diagnosed with Ehlers Danlos Syndrome a rare genetically inherited connective tissue disorder and associated POTS. As I have 4 ruptured relatives mine is thought to be type IV, the Vascular Type. Went onto 5g sodium a day to better manage autonomic episodes (common self management with POTS/Dysautonomia).
- Diagnosed with Diverticular Disease which is common in EDSIV.
PSYCHIATRIC
- (1979-1980) Hospital outpatient for mood and anxiety disorders
- (1983) 6 months Gestalt therapy for PTSD
- (1990) 3 months counseling for PTSD
- (1996) 6 months grief counseling after my father died
- (1997-2002) CBT for mood, anxiety, compulsive disorders and PTSD
- (2001-2004) Risperdal 0.5mg for mood, anxiety and compulsive disorders
- (2004-2011) Changed to 25-50mg Seroquel for mood, anxiety and compulsive disorders
- (2010) Diagnosed with Dissociative Identity Disorder (DID) (by a psychiatrist who I'd met for the first time) during a medication review. However, autism expert Lawrie Bartak (who has known me since 1991) says what may be diagnosed as DID in a non autistic person may be a common coping strategy in girls on the autism spectrum.
- (2011) Went legume free (IgE soy/peanut allergies) then off Seroquel- no complications
- (2010-2015) CBT for PTSD and DID
 |
NOTE: Contrary to the extensive, and often emotive public ignorance about the condition, DID is not a personality disorder. It is listed in the DSMV as a condition within the spectrum of DISSOCIATIVE Disorders on the same spectrum as Post Traumatic Stress Disorder (PTSD) and can co-occur in ANY severely traumatised human being alongside any Developmental Disability or health condition they already have.
Dissociative symptoms can coexist with other childhood psychiatric conditions (R1555256AA). In fact, an underlying mood disorder, cognitive disorder, or pervasive developmental disorder may lower a child's threshold for coping with a traumatic environment and therefore make the child more vulnerable to the development of comorbid dissociative symptoms. (http://ajp.psychiatryonline.org/article.aspx?articleid=172850)
"Dissociation can be defined on a continuum. On one end try to imagine yourself driving down the highway. Suddenly you have arrived at your destination but you cannot recall how you got there. This is a form of mild dissociation and everyone does this. On the opposite end you would find dissociation defined as multiplicity which is now known as DID (Dissociative Identity Disorder). DID is not an illness nor is it a disease. The individuals that have been diagnosed with this disorder are not crazy. They are survivors of severe childhood trauma and the long-term effects have caused these individuals problems on how to process current information and react to everyday life". (from PsychCentral.com)
 |
DID I LOOK AUTISTIC?
Not sure what 'autistic' looks like, but an extensive photographic history of my development (most pics there were taken by my Paternal uncle who was a photographer) from the age of about 1 month old to the age of 14 and beyond can be viewed at any time.
TAKING 'SHIT' AND MAKING 'SCULPTURES'
As a Taoist, I find the positives in otherwise negative experiences.
Had I not been so 'voiceless', and so 'silenced', I would probably not have continued to write books after my third one. Instead I have ten published books including 4 text books used in training in special education and psychology courses around the world. Without feeling so useless and hopeless I would probably not have worked so hard to focus on what use I could be to the world or put all my energies into the consulting work I did since 1996, having now worked to bring hope to over 1000 families of children on the autism spectrum in countries around the world. Without having suffered for the ignorance about my autism, I would not have been driven to build better awareness about autism and challenge the now laughable presumptions and stereotypes that surround it. Without becoming a 'controversy', I would never have bothered to disclose so much personal diagnostic detail and complete pictorial history which has benefited the autism world as one of the most complete online diagnostic and pictorial histories of any well known person diagnosed with autism. For these things, I am grateful for the 'shit', and for the 'sculptures' I made from it.